Seeking information about the stomach and stomach cancer can feel overwhelming or frightening, especially if you’re unsure about what’s ahead for you or a loved one. Having the right information can help lessen some of these feelings. Here you will find reliable information about the stomach and stomach cancer along with diagnosis, symptoms, risks, treatment, side effects, diet and nutrition and some useful websites to visit.
Nau mai rā, rarau mai rā ki tēnei whārangi mō ngā kōrero e pā ana ki te mate pukupuku puku.
About the stomach
Mō te puku
The stomach is part of the digestive system. The stomach is a hollow muscular sack like organ that receives and stores food from the oesophagus (food pipe).
It has a sphincter (valve) at each end and is located on the upper left side of your abdomen. Its function is to store food while it is being mixed with stomach enzymes that breaks food down into a thick liquid and secretes a strong acid that kills any bacteria that entered with the food or drink.
When the contents of the stomach are processed enough, they are released into the small intestine where nutrients are absorbed into the bloodstream.
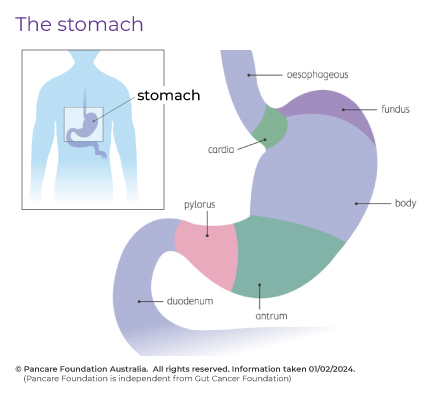
Click here to view a diagram of the stomach | Pāwhirihia ki kōnei kia tirohia he hoahoa whakaahuahanga o te puku
cardia: the first part is closest to the oesophagus
fundus: the upper part of the stomach
body: the main part of the stomach
antrum: the lower portion (near the intestine), where the food mixes with gastric juice
pylorus: the last part of the stomach, which acts as a valve to control emptying of the stomach contents into the small intestine.
Learn more about the stomach and symptoms of the cancer
This video contains sensitive images of organs and the body
What is stomach cancer? | He aha tēnei mea te mate pukupuku puku?
Stomach cancer occurs when abnormal cells grow out of control. Also known as gastric cancer, there are several different types of stomach cancer.
Click on each type of cancer below to learn more about them | Pāwhirihia kia whai mōhiotanga mō ia momo mate pukupuku i raro iho nei.
Adenocarcinoma
About 95% of stomach cancers develop in the cells that line the inside surface of the stomach and are called gastric adenocarcinomas.
Lymphomas
Cancer of specialised cells that are part of the immune system. These can arise in the stomach or other parts of the digestive tract.
Gastro-Intestinal Stromal Tumours (GISTs)
Cancer arising from pacemaker cells that control stomach wall muscle contractions. GISTs can also develop in other parts of the digestive tract but most frequently occur in the stomach.
Carcinoid tumours (also known as neuroendocrine tumours or NETs)
Cancer of hormone-producing cells. These can arise in the stomach as well as in other parts of the digestive tract.
The main form of stomach cancer (adenocarcinomas) can sometimes be split into two sub-types; intestinal and diffuse-type however often tumours are a mix of subtypes where there is a combination of both features. A classification is made by a pathologist.
Intestinal stomach cancer | Mate pukupuku puku kōpiro
Intestinal stomach cancer is linked to a number of environmental factors such as Helicobacter pylori (H. pylori) infection, smoking and salt-preserved foods. It can sometimes be the result of an inherited genetic mutation passed down through family and whānau.
Diffuse-type stomach cancer | Mate pukupuku momo hora
Hereditary stomach cancer is cancer that is caused by a mutation in a particular gene that is passed down through family and whānau. This type of hereditary mutation usually causes diffuse-type stomach cancer. The level of hereditary diffuse-type stomach cancer in New Zealand is much higher than in many other countries. There has been excellent research led by Professor Parry Guilford (Te Aho Matatū), Associate Professor Karyn Paringatai and driven by Maybelle McLeod (Kimihauora Health and Research Clinic) into the CDH1 gene mutation and its impact on whānau and how understanding whakapapa can help identify those most at risk.
Diffuse-type stomach cancer can also be associated with environmental factors such Helicobacter pylori (H. pylori) infection. It can be linked to hereditary gene mutations that is caused by a mutation in a particular gene (CDH1) that is passed down through family and whānau and is more common in Māori and Pacific people. This type of hereditary mutation usually causes diffuse-type stomach cancer.
Stomach cancer statistics in New Zealand | Ngā tauanga mate pukupuku puku i Aotearoa
Stomach cancer in New Zealand has some of the largest inequities for our Māori and Pasifika populations who are 3 times more likely to develop the disease than NZ Europeans.
Click here to read more about these inequities | Pāwhirihia ki kōnei kia pānui i ētahi kōrero āpiti mō ngā tautika-kore
The increased likelihood of developing stomach cancer for Māori and Pasifika populations is linked to two main factors:
Mate pukupuku puku kōpiro | Intestinal-type Stomach Cancer is linked to a number of environmental factors that Māori and Pasifika communities are more exposed to such as Helicobacter pylori (H. pylori) infection, smoking and salt-preserved foods.
Mate pukupuku momo hora | Diffuse-type stomach cancer is linked to hereditary gene mutations, such as the CDH1 mutation, which are far more prevalent in Māori whānau.
The level of hereditary diffuse-type stomach cancer in New Zealand is much higher than in many other countries. There has been excellent research led by Professor Parry Guilford (Te Aho Matatū), Associate Professor Karyn Paringatai and driven by Maybelle McLeod (Kimihauora Health and Research Clinic) into CDH1 gene mutations and the impact on whānau and how understanding whakapapa can help identify those most at risk.
The prevalence of a CDH1 gene mutation among some Māori whānau accounts for between 20-50% of these cases, but the cause of the rest remains unknown. This means New Zealand has unique epidemiology around stomach cancer that needs to be researched further to ensure we can identify those New Zealanders at most risk and are giving New Zealanders appropriate treatment options. Click here to find out more about Hereditary Diffuse Stomach Cancer
Read our opinion piece about stomach cancer in New Zealand
Symptoms & Risks
Tohumate & Tūraru

Symptoms of stomach cancer | Ngā tohumate o te mate pukupuku puku
The symptoms of stomach cancer are often vague and non-specific. They are often subtle and occur in other medical conditions apart from stomach cancer, making them difficult to link to stomach cancer. Stomach cancer symptoms vary widely.
It is important to note that having one or more of these symptoms does not necessarily mean that you have cancer, but if you have new or persistent symptoms that are out of the ordinary for you, it’s really important that you contact your GP to get checked out.
Download our symptoms tracker if you'd like something to take to your GP appointment to guide a conversation about symptoms.
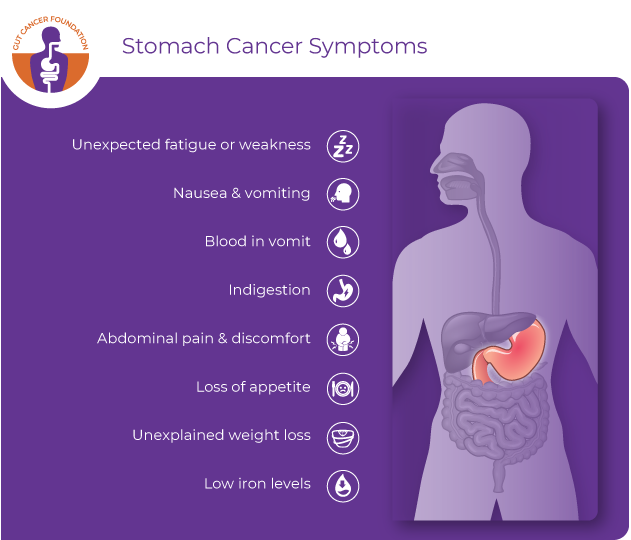
Click here to view symptoms of stomach cancer | Pāwhirihia ki kōnei kia tirohia ngā tohumate o te mate pukupuku puku.
Stomach Cancer symptoms may include:
a painful or burning sensation in the abdomen
heartburn or indigestion (dyspepsia)
a sense of fullness, even after a small meal
nausea and/or vomiting
loss of appetite and/or weight loss
swelling of the abdomen
unexplained tiredness or weakness
low iron levels, red blood count/ anaemia
blood in vomit
black-coloured stool.
It is best to see your doctor for review and investigation if you experience unexplained symptoms that worry you. They will ask you questions to help understand whether the cause of symptoms is stomach cancer or another condition.
Managing symptoms | Whakahaere i ngā tohumate
You might notice that things change for you physically and emotionally following your diagnosis and you may have even noticed some of these symptoms prior to diagnosis. Understanding them can help you to prepare for them mentally and manage them if they do appear.
If you do experience any of these symptoms, let your healthcare team know when you next see them. If they are extreme, or you are worried about them, get in touch with your healthcare team sooner.
Click below to learn about some ways you can manage these changes or symptoms | Pāwhirihia te momo tohumate mō ētahi atu mōhiohio.
Changes in diet | Ngā panonitanga o te whiringa Kai
Many people find that sorting out symptoms related to their diet makes the biggest difference to how they feel. Ask your doctor or nurse for a referral to a dietitian. They can help you with finding food to eat that is gentle on your digestive system.
Nausea | Whakapairuaki
Feeling sick (nauseous) is another common symptom. You may be prescribed anti-sickness medication, or you could try home remedies such as ginger, peppermint, or acupressure bracelets.
Fatigue | Ruha
You are bound to feel tired or exhausted sometimes, so be kind to yourself. Make sure you rest and prioritise what you want or need to do. Give yourself permission to accept offers of help for chores that feel overwhelming. Although you might not feel like it, gentle exercise such as stretching, or a short walk can help combat fatigue.
Intimacy | Mateoha
People of all genders can lose interest in sexual activity during cancer treatment, at least for a time. Although it can feel awkward, talking to your partner about what you find intimate, or soothing can help. There are many ways to be intimate, such as cuddling or gentle touch, or using warmth and comforting language. Your GP may be able to assist with medication or a referral to see a sex and relationship therapist.
Stress, pain, and anxiety | Kohuki, Mamae, Anipā
Simple relaxation techniques can help you cope with stress, pain, and anxiety. Having a warm bath, deep breathing or listening to soothing music are easy things to do at home. You might want to try complementary therapies like reflexology or aromatherapy massage. Talking to others can also help. There are many cancer-specific psychologists available to you in New Zealand – ask your oncologist, nurse, or GP for a referral.
Keep perspective | Kia whakataurite
Each individual will feel and react differently to treatment. What might work for someone else may not always work for you. Acknowledge that not every day will be as easy to manage as the last, and that every day may be different. Focus on what you know works for you and be very gentle with yourself.
Keeping active | Kia kori
Physical activity can also make you feel better, though how much activity will depend on how well you feel. Even a walk round the block or 10 minutes of stretching each day can help.
Risks of developing stomach cancer | Ngā tūraru whakawhanake mate pukupuku puku
There are some known risk factors that can increase the chance of stomach cancer developing. Having a risk factor does not automatically mean that you will develop stomach cancer, but they do increase the likelihood of it happening.
Knowing your risk factors and talking about them with your doctor may help you make more informed lifestyle and health care choices.
Some risk factors are environmental and within your control which is why it is important to understand what they are.
Risk factors that cannot be controlled | Ngā pūtake tūraru here kore
Age | Pakeke
Stomach Cancer can occur in younger people, but the risk goes up as a person gets older. Most people diagnosed with stomach cancer are in their 60s, 70s, or 80s. (However, people with a family history, in particular Māori, can be impacted at a much younger age).
Gender | Ira
Stomach cancer is more common in men than in women.
Ethnicity | Mātāwaka
Māori & Pacific Island communities are at higher risk of stomach cancer than NZ Europeans.
Family history of gastrointestinal cancers | Kōrero hītori whānau
Hereditary stomach cancer is cancer that is caused by a mutation in a particular gene that is passed down through family and whānau. This type of hereditary mutation usually causes diffuse-type stomach cancer. The level of hereditary diffuse-type stomach cancer in New Zealand is much higher than in many other countries. There has been excellent research led by Professor Parry Guilford (Te Aho Matatū), Associate Professor Karyn Paringatai and driven by Maybelle McLeod (Kimihauora Health and Research Clinic) into the CDH1 gene mutation and its impact on whānau and how understanding whakapapa can help identify those most at risk.
Genetics | Huaira
Inheriting a genetic mutation that causes bowel disorders, familial adenomatous polyposis (FAP) or hereditary nonpolyposis colorectal cancer (HNPCC). the CDH1 genetic mutation is an example of this.
Societal and environmental risk factors that can be controlled | Ngā pūtake tūraru-ā-porihanga, ā-taiao whai here
Helicobacter pylori infection | Poke h pylori
Infection with Helicobacter pylori (H pylori) bacteria seems to be a major cause of stomach cancer, especially cancers in the lower (distal) part of the stomach. Long-term infection of the stomach with this germ may lead to atrophic gastritis and other pre-cancerous changes of the inner lining of the stomach.
People with stomach cancer have a higher rate of H pylori infection than people without this cancer. H pylori infection is also linked to some types of lymphoma of the stomach. Even so, most people who carry this germ in their stomach never develop cancer.
H. pylori, a group 1 carcinogen, causes nearly 90% of non-cardia gastric cancers, with the lifetime risk of developing gastric cancer of approximately 3 percent in those infected. Māori and Pacific people have a higher prevalence of H. pylori infection when compared with NZ Europeans. H. pylori infection rates are 35% in Māori, 62% in Pasifika and 18% in NZ Europeans as well. Māori and Pasifika are also infected with a more carcinogenic strain. These ethnic differences in H. pylori are the predominant reason for the inequities that exist in gastric cancer rates and deaths between Māori and NZ European in Aotearoa.
Identifying and treating H. pylori can prevent the development of stomach cancer. While patients with symptoms such as dyspepsia should be tested for H. pylori, infection is often asymptomatic. This highlights the importance of opportunistic testing of individuals at elevated risk of infection. These risk factors include:
Patient is in a high-risk population: Māori or Pasifika
A family member has tested positive for H. Pylori
Being overweight or obese | Pukunati
Being overweight or obese is linked with an increased risk of cancers of the cardia (the upper part of the stomach near the oesophagus).
Diet | Whiringa kai
Stomach Cancer risk is increased in people whose diets include large amounts of foods preserved by salting, such as salted fish and meat and pickled vegetables. Eating processed, grilled, or charcoaled meat regularly appears to increase the risk of non-cardia stomach cancers. Eating few or no fruits likely increases the risk of stomach cancer. On the other hand, eating lots of fresh fruits (especially citrus fruits) and raw vegetables appears to lower the risk of stomach cancer.
Alcohol use | Inu waipiro
Alcohol use is likely to increase the risk of stomach cancer. The evidence for this link is strongest for people who have 3 or more drinks per day.
Tobacco use | Momi tūpeka
Smoking increases the risk of stomach cancer, particularly for cancers of the upper part of the stomach near the oesophagus. The likelihood of developing stomach cancer is about double in people who smoke.
Diagnosis
Tautohunga
Diagnosing stomach cancer | Te tautohunga i te mate pukupuku puku
Being diagnosed with cancer can be a scary time for anyone. Here you will find information to help you understand some of the terms you might have heard.
In order to diagnose stomach cancer, your treatment team will do a range of tests. There might be one test or a mix of tests, some of which are explained below.
Clinical examination
If you have symptoms of stomach cancer, your doctor may carry out a general clinical examination. The doctor will ask about your medical history to learn about your symptoms and possible risk factors.
Blood Tests | Whakamātau toto
Blood tests are sometimes taken to check your liver function (LFT) and full blood count (FBC) for overall health. The FBC tells the doctor if you have a low red blood cell count which sometimes happens if the tumour has been bleeding. Blood tests provide useful information, but they cannot be used alone to diagnose stomach cancer.
A Faecal Occult Blood test (FOBT) is a stoll test and may be done to look for blood in stool (faeces) that can’t be seen by the naked eye (which could be caused by the cancer bleeding into the stomach).
Endoscopic ultrasound (EUS) | Oro ikeike tiro oranga whekau
An endoscopic ultrasound uses a flexible tube with a camera on it (called an ‘endoscope’) which is inserted into the mouth and oesophagus (food pipe). It uses sound waves to create images. Sometimes, there is a small needle on the end that can take fluid or tissue samples (a biopsy) that can be analysed later by the lab.
An EUS can help a doctor see a tumour’s location and size, check whether the cancer has spread to other nearby areas of the body. The images provided by this internal ultrasound have been shown to be helpful in determining whether a tumour can be removed with surgery.
During an upper EUS test, you lie on your left side. A healthcare provider:
gives you an IV sedative to help you relax
sprays your throat with a numbing medicine
places a plastic mouthguard in your mouth. The mouthguard protects your teeth and prevents you from biting down on the endoscope
inserts the ultrasound endoscope through your mouth and into the oesophagus
you shouldn’t feel any pain and you will be able to breathe as usual
when the images and/or biopsy have been taken, the healthcare provider gently removes the endoscope and stops anaesthesia. You slowly wake up in a recovery room.
An EUS takes about 1 hour and occurs in an outpatient setting. As you will receive a sedative you will need to take someone with you who can drive you home and stay with you for the remainder of the day.
To prepare for your EUS you may be asked to:
adjust the dosage of your medications such as blood thinners or insulin as recommended by your provider
not eat or drink for a set period of time before the test.
take off your clothes on your upper body and change into a hospital gown.
Endoscopic ultrasounds are a very safe procedure, but sometimes minor complications may occur. These include:
Sore throat
A small amount of bleeding if a biopsy has been taken
Bloating – as air is sometimes pumped through the endoscope during the procedure
Small tear in the throat – from insertion of the endoscope
Fluid on the lungs – if fluid from your mouth went into the lungs during your procedure
Shortness of breath – due to the effects of the sedative
Upper endoscopy | Tiro oranga whekau runga
During an upper endoscopy, you are sedated (made sleepy) and then the doctor passes an endoscope down your throat and into the oesophagus. The endoscope’s camera is connected to a monitor, which lets the doctor see any abnormal areas in the wall of the oesophagus clearly. The doctor can take tissue samples from any abnormal areas. These samples are sent to the lab to check if they contain cancer.
If oesophageal cancer is found and is blocking the oesophagus, certain instruments can be used to help enlarge the opening (dilate) to help food and liquid pass. Upper endoscopy can give the doctor important information about the size and spread of the tumour, which can be used to help determine if the tumour can be removed with surgery.
Computed tomography (CT) scan | Matawaitanga-ā-rorohiko
A computerised tomography scan (CT scan) combines a series of x-ray images that are taken from different angles around the body. You will lie on a motorised bed that passes through a doughnut shaped tube. It is important that you lay still for good quality images to be taken and so a strap and/or pillows may be used to help with this. It isn’t painful and usually takes about 1 hour in an outpatient setting.
Hei whakarite i mua i te whakaata roto ka pātaihia pea i ēnei pātai | To prepare for the scan, you may be asked to:
stop eating or drinking for 4 hours before your scan
take off some or all of your clothing and wear a hospital gown for the scan
remove all objects such as jewellery, piercings, dentures, and glasses as they will interfere with the picture quality.
most patients will receive contrast which requires an IV line. Contrast allows for organs in question to be seen clearly.
A CT scan uses small amounts of radiation. This is greater than the amount you would get during a simple x-ray, however it is still a small amount and so the risk to your health is very low. The low dose of radiation you are exposed to during a CT scan has not been shown to cause harm.
Click here for an example of an CT scan.
Ultrasound | Oro ikeike
Ultrasound scans use a microphone (probe) that gives off sound waves to provide an image on a computer of the inside of your body. Some gel is put on your tummy and the probe is moved over the gel with a little pressure. Sometimes you may have a contrast dye injection before your scan that will help to show any growths clearly.
Click here for an example of an Ultrasound.
Magnetic resonance imaging (MRI) | Whakaahua ponguru autō
An MRI scan uses magnet fields and radio waves to produce a detailed picture of the body. You will lie on a bed that moves into a tube. It is important that you lay still for good quality images to be taken. It isn’t painful and usually takes between 15 and 90 minutes in an outpatient setting. An MRI scan is very noisy and so you may be given headphones to wear. For those who do not like small spaces it may cause some anxiety. If this is the case, speak to your doctor before your MRI as they may be able to provide you with some relaxation tips or medicine to help you feel calmer.
To prepare for the scan | Hei whakarite i mua i te whakaata roto:
you may be asked to stop eating a few hours before the scan but will be informed beforehand if this is the case
take off some or all of your clothing and wear a hospital gown for the scan
remove all metal objects such as hair clips and piercings and possibly medical patches if you wear one as they may contain metal.
It is important to tell the radiology staff about any metal you have in your body including possible metal fragments in your eye and metal foreign bodies. Objects that have been implanted in your body need to be discussed ahead of the MRI scan as they may cause harm or be damaged. These include pacemakers, aneurysm clips, heart valve replacements, neurostimulators, cochlear implants, magnetic dental implants, and drug infusion pumps.
Click here for an example of an MRI
Laparoscopy | Poka mātai papatoiake
Laparoscopy is usually only done after stomach cancer has already been found. A laparoscopy can help doctors check that the cancer is still only in the stomach before undertaking surgery.
Laparoscopy is undertaken in an operating theatre in hospital and you will be given a general anaesthetic (you will be in a deep sleep). A laparoscope (a thin, flexible tube) is inserted through a small surgical opening in your side. The laparoscope has a small video camera on its end, which sends pictures of the inside of the abdomen to a TV screen. Doctors can look closely at the surfaces of the organs and nearby lymph nodes, or even take small samples of tissue.
Click here to view an example of a laparoscopy | Pāwhirihia ki kōnei kia tirohia he hoahoa whakaahuahanga o te laparoscopy
Positron emission tomography (PET) | Matawaitanga-ā-rorohiko whakarau pūngao
Although not commonly used to diagnose gastric cancer, It can be required in certain situations. A PET scan uses a special type of camera that detects radioactive material. A small amount of radioactive material is injected into your arm about 1 hour before the scan which will travel and accumulate in areas of the body where there is higher metabolic activity i.e., where there is disease occurring. The body is then scanned to show where the radioactive material is accumulating.
Allergic reactions can occur due to the radioactive material but are extremely rare.
Similar to the CT scan, you will lie on a motorised bed that passes through a doughnut shaped tube. Sometimes the CT scan and PET scan are combined in the same machine and both types of images are taken at the same time. It is important that you lay still on the bed for good quality images to be taken and so a strap and/or pillows may be used to help with this. It isn’t painful and the whole procedure usually takes about 2 hours in an outpatient setting.
After the procedure you naturally pass the radioactive material out of your body in your urine.
To prepare for the scan you may be asked to | Hei whakarite i mua i te whakaata roto ka pātaihia pea i ēnei pātai:
avoid strenuous exercise for a couple of days before
stop eating 4 hours before your scan.
Click here for an example of a PET scan.
Barium x-rays | Whakamātau horomi waitāmura me te whakaata roto
In this test, you will be asked to swallow a thick, chalky liquid called barium. The barium coats the lining of the oesophagus, stomach, and small intestine. Several X-ray pictures are then taken. Because X-rays cannot pass through the coating of barium, this will outline any abnormalities of the lining of these organs.
It's important to acknowledge that some of these tests can be confronting or sometimes frightening. Taking a friend or whānau member with you can help ease anxiety. Be encouraged to tell staff if you need extra reassurance during the test, you'll find some very compassionate people working in healthcare.
Waiting to have tests carried out | E tāria ana kia whakamātauhia
Even if you have been given an urgent referral for a particular scan or investigation you may have to wait several days or possibly weeks for your appointment. This can be frustrating and worrying, especially if you are already feeling unwell.
Several weeks of testing to confirm a diagnosis or awaiting appointments is relatively common and is unlikely to alter overall outcomes. Cancer growth is considered to be negligible over a period of weeks, and this waiting period is unlikely to cause you harm if your symptoms are stable.
If your symptoms get worse or you start to feel more unwell while you are waiting, it is a good idea to get in touch with your GP or specialist if you already have one. If you cannot get in contact with them, you may need to present to the closest emergency department if your symptoms cannot be controlled at home.
How long will I have to wait for my test results? | Ka hia te roa e tatari ai kia puta ngā kitenga whakamātautau?
Depending on which tests you have had it may take from a few days to a few weeks for the results to come through. Waiting for test results can be an anxious time.
It is a good idea to ask how long you may have to wait when you go for tests. If you think you have been waiting too long, then contact your GP or a specialist to follow up on the progress of your results. Usually, the doctor who does the test will write a report and send it to your specialist. If your GP sent you for the test, the results will be sent to the GP clinic.
You will need an appointment with your specialist or GP to discuss the test results and how they might affect your treatment. Usually, your specialist will discuss your results and plan your subsequent care.
All these tests will give the specialist more information about the cancer such as where it is, if it is growing, and if it has spread. This is called staging. Staging helps to work out the best treatment plan for you.
Stomach cancer stages | Ngā tūātupu o te mate pukupuku puku
You may have heard people talk about the stages of cancer. Staging provides an indication of the size of the cancer and if it has spread to other areas of the body and contributes to the treatment planning.
There are two ways in which the stage of cancer can be described. One uses numbers (stage 1, 2 etc) and the other uses letters and numbers (T1, N0, M0 etc) also known as TNM (Tumour-Nodes-Metastases) staging. The cancer may be described in one or both ways by your healthcare team.
Click here to learn more about the stages of cancer | Pāwhirihia kia whai mōhiotanga mō ngā tūātupu mate pukupuku.
TNM (Tumour-Nodes-Metastases) staging | Te Tūātuputanga Pukupuku, Tīpona, Hora-mate
The TNM gives a number according to tumour size (T), how many lymph nodes are affected (N), and how far the cancer has spread, or metastasised, to distant parts of the body (M). This may be expressed as, for example, T1, N0, M0. This information is used to help decide the best treatment.
Tis | Cancer only found in cells on the surface of the lining of the stomach and has not spread to other layers of the stomach. | |
T1 | Tumour has grown into inner layers of the wall of the stomach (the lamina propria, muscularis mucosae, or the submucosa). | |
T2 | Tumour has grown into the muscle layer of the stomach (the muscularis propria). | |
T3 | Tumour has grown through all of the layers of the muscle into the connective tissue outside the stomach. It has not grown into the lining of the abdomen, called the peritoneal lining, or into the serosa, which is the outer layer of the stomach. | |
T4 | Tumour has grown through all of the layers of the muscle into the connective tissue outside the stomach. It has also grown into the peritoneal lining or serosa or the organs surrounding the stomach. | |
N1 | 1-2 lymph nodes involved | |
N3 | 7 or more lymph nodes involved | |
M1 | Distant metastasis |
Staging using numbers | Te tūātuputanga mahinga tau
Stage 1 | The earliest stage when cancer is found only in the stomach lining. |
Stage 2 | The cancer has spread deeper into the layers of the stomach. |
Stage 3 | The cancer has spread to nearby lymph nodes, known as locally advanced disease. |
Stage 4 | The cancer has spread to other parts of the body (metastatic cancer) such as the liver, lungs, distant lymph nodes or to the tissue lining the abdominal cavity (peritoneum). |
Prognosis (Life expectancy) | Matapaenga (Te wā ora)
Like any cancer there are many things that can impact on survival rates, so it is best to talk to your cancer specialist for guidance about your own care and outcomes. Remember, even with a diagnosis, no one can know for certain how long anyone will live. Estimates of life expectancy are based on historical data, however treatments are becoming more effective over time which changes these estimates.
Prognosis is usually improved the earlier the cancer is detected. Your doctor will be able to give you the best idea of prognosis.
Often, statistics talk about survival rates which are taken from an average of other patients. These are usually described in 1, 5 and 10-year survival rates. A 10-year survival rate is the proportion (or percent) of people who have not died 10 years after having cancer, however many people live much longer than this.
Stomach cancer statistics in New Zealand | Ngā tauanga mate pukupuku puku i Aotearoa
Stomach cancer in New Zealand has some of the largest inequities for our Māori and Pasifika populations who are 3 times more likely to develop the disease than NZ Europeans.
Click here to read more about these inequities | Pāwhirihia ki kōnei kia pānui i ētahi kōrero āpiti mō ngā tautika-kore
The increased likelihood of developing stomach cancer for Māori and Pasifika populations is linked to two main factors:
Mate pukupuku puku kōpiro | Intestinal-type Stomach Cancer is linked to a number of environmental factors that Māori and Pasifika communities are more exposed to such as Helicobacter pylori (H. pylori) infection, smoking and salt-preserved foods.
Mate pukupuku momo hora | Diffuse-type stomach cancer is linked to hereditary gene mutations, such as the CDH1 mutation, which are far more prevalent in Māori whānau.
The level of hereditary diffuse-type stomach cancer in New Zealand is much higher than in many other countries. There has been excellent research led by Professor Parry Guilford (Te Aho Matatū), Associate Professor Karyn Paringatai and driven by Maybelle McLeod (Kimihauora Health and Research Clinic) into CDH1 gene mutations and the impact on whānau and how understanding whakapapa can help identify those most at risk.
The prevalence of a CDH1 gene mutation among some Māori whānau accounts for between 20-50% of these cases, but the cause of the rest remains unknown. This means New Zealand has unique epidemiology around stomach cancer that needs to be researched further to ensure we can identify those New Zealanders at most risk and are giving New Zealanders appropriate treatment options. Click here to find out more about Hereditary Diffuse Stomach Cancer
Click here to view stomach cancer statistics related to morbidity (number of diagnoses) and mortality (survival rate). Remember that everyone is different, and statistics are only a guide. | Pāwhirihia kia tirohia ngā tauanga tahumaero me te matenga ā te Mate pukupuku puku.
This includes a small number of people with gastro-intestinal stromal tumours (GIST) and neuroendocrine tumours (NETs).
Stomach cancer is one of the cancers with the greatest inequities for Māori when compared with non-Māori. Māori are 3 times more likely to develop stomach cancer than NZ European communities and are over 3.5 times more likely to die from the disease.
The prognosis after treatment depends on the stage and the treatment given. In the best circumstances, cure is possible. If cure is not possible, the symptoms caused by the cancer can often be alleviated.
Overall, the survival rate for stomach cancer is 44.1% at year one, 22.7% at year 5, and 20.7% at year 10. Around 274 New Zealanders die from stomach cancer each year.
Remember that everyone is different, and statistics are only a guide.
Treatment
Ngā momo rongoā

Treatment Options | Ngā kōwhiringa rongoā
There are a number of treatment options available, and it may feel confusing and unsettling not knowing which will be the best for you. Treatment of stomach cancer depends on its location, the stage of the cancer (how advanced it is at the time of diagnosis), and whether the person is otherwise medically fit.
The choice of treatments will be discussed with you and your whānau and your preferences will be considered. Your treatment will be discussed by a multidisciplinary team (MDT), which means that experts in different areas of cancer treatment (e.g., surgeons, gastroenterologists, pahologists, radiologists, oncologists, and nurses) come together to share their expertise in order to provide the best patient care.
It is also important to note that more than one treatment may be needed to get the best results.
Surgery to remove part or all of the stomach is the most common curative treatment, but radiotherapy and chemotherapy may also be used.
See below to read more about the treatment options.
*Not all the options below will be applicable to everyone's situation. Some treatments listed may not be funded and would require the patient to pay directly. It is important to discuss all your options with your specialist team.
Surgery | Poka tinana
Once the diagnosis is made, surgery to remove the cancer where possible is the best treatment option in the majority of cases. The aim of surgery may be to remove the cancer, part or all the stomach and some nearby lymph nodes, depending on the type and stage of stomach cancer.
The type of surgery usually depends on what part of the stomach the cancer is in and how much cancer is in the surrounding tissue. Different kinds of surgery can be used to treat stomach cancer.
Endoscopic mucosal resection:
Endoscopic submucosal resection can be used to treat only some very early-stage cancers in which the chance of spread to the lymph nodes is very low. In an endoscopic resection, the surgeon passes an endoscope (a long, flexible tube with a small video camera on the end) down the throat and into the stomach. Surgical tools can be passed through the endoscope to remove the tumour and part of the normal stomach wall around it.
Subtotal (partial) & total gastrectomy:
Subtotal (partial) gastrectomy
This operation is when part of the stomach is removed, sometimes along with part of the oesophagus or the first part of the small intestine (the duodenum). The remaining section of stomach is then reattached. Some of the omentum (an apron-like layer of fatty tissue that covers the stomach and intestines) is removed as well, along with nearby lymph nodes, and possibly the spleen and parts of other nearby organs.
Eating is much easier after surgery if only part of the stomach is removed instead of the entire stomach
Total gastrectomy
This operation is done if the cancer has spread throughout the stomach. It is also often advised if the cancer is in the upper part of the stomach, near the oesophagus. It is also advised if someone has a familial cancer syndrome such as Hereditary Diffuse Gastric Cancer (HDGC) due to a CDH1 genetic mutation.
The surgeon removes the entire stomach, nearby lymph nodes, and omentum, and may remove the spleen and parts of the oesophagus, intestines, pancreas, or other nearby organs. The end of the oesophagus is then attached to part of the small intestine. This allows food to move down the intestinal tract. But people who have had their stomach removed can only eat a small amount of food at a time. Because of this, they must eat more often.
Most subtotal and total gastrectomies are done through a large cut in the skin of the abdomen. In some hospitals, this can be done using laparoscopy, which allows the stomach to be removed through several smaller cuts in the abdomen.
Read about Carl Sunderland's experience of a total gastrectomy here
Feeding tube placement
Some patients have trouble taking in enough nutrition after surgery for stomach cancer. Further treatment like chemotherapy with radiation can make this problem worse. To help with this, a tube can be placed into the intestine at the time of gastrectomy. The end of this tube, called a jejunostomy tube or PEJ tube, remains outside of the skin on the abdomen. Through this, liquid nutrition can be put directly into the intestine to help prevent and treat malnutrition.
Interventions for unresectable cancer | Ngā hāpaiora mō te mate pukupuku taunoho
For people with unresectable stomach cancer (i.e., not capable of being surgically removed) surgery can often still be used to help control the cancer or to help prevent or relieve symptoms or complications.
For people with unresectable stomach cancer (i.e., not capable of being surgically removed) surgery can often still be used to help control the cancer or to help prevent or relieve symptoms or complications.
Endoscopic tumour ablation
In some cases, such as in people who are not healthy enough for surgery, an endoscope (a long, flexible tube passed down the throat) can be used to guide a laser beam to vapourise parts of the tumour.Stent placement
Another option to keep a tumour from blocking the opening at the beginning or end of the stomach is to use an endoscope to place a stent (a hollow metal tube) in the opening. This helps keep it open and allows food to pass through it.
Chemotherapy | Haumanu matū
Chemotherapy uses drugs to kill cancer cells and stop the cancer growing and dividing.
Chemotherapy is a drug which is administered either by swallowing tablets; through an injection; or through infusion which is a small tube that is inserted into a vein. The drug works by moving through the blood stream to kill the cancer cells. Unfortunately, some healthy cells can also be harmed leading to side effects. Chemotherapy can be given alone or in combination with other therapies such as targeted therapy, surgery, or radiation. It is usually administered in an outpatient clinic and sometimes a hospital stay is needed if the doctor wants to monitor you following treatment.
Chemotherapy is commonly given before surgery for stomach cancer to shrink large tumours and destroy tumours that may have spread. It is also used when tumour removal is achieved, to reduce the risk of the cancer returning.
Click here to view an example of chemotherapy infusion | Pāwhirihia ki kōnei kia tirohia te hoahoa whāuru haumanu matū.
Radiation therapy | Haumanu iraruke
Radiation therapy may be used as a stand-alone treatment or in conjunction with surgery and/or chemotherapy. Radiotherapy is often used in stomach cancer to shrink the tumour, relieve symptoms, and help you feel more comfortable. It is used to control symptoms such as pain and bleeding when surgery is not suitable.
Radiation therapy uses x-rays (ionising radiation) to damage the deoxyribose nucleic acid (DNA) of cancerous cells to kill the cancer cells and stop the cancer growing. It can be given for all stages of cancer.
External beam radiation therapy | Haumanu Iraruke pūhihi rāwaho
Getting radiation therapy is similar to getting an X-Ray but the radiation is stronger. It is a painless procedure which involves lying on a table and a large machine rotating around you. It is directed at the tumour to try to kill the tumour or stop the cancer cells growing without damaging the healthy tissue nearby. Radiotherapy is usually performed in an outpatient clinic. It usually takes place everyday Monday to Friday and lasts for about 10-20 minutes. Your treatment team will be able to tell you how many weeks you will need radiotherapy for.
Click here to view view an example of external beam radiation therapy.
Clinical trials | Whakamātau haumanu
You may be eligible to take part in a clinical trial, which is a type of research study that investigates new or specialised therapies or treatments. While you are discussing therapy options with your care team, it is a good idea to ask about clinical trials that may be suitable for your condition and discuss whether participating may be right for you.
Being involved in a clinical trial may be beneficial in that you may access the latest treatments before they become generally available. Additionally, clinical trial participation is often associated with closer monitoring of your care and condition and potentially improved outcomes.
Click here to learn more about clinical trials | Pāwhirihia ki kōnei kia tirohia tētahi tauira o te whāuru haumanu matū.
Palliative care | Pairuri
A specialist may refer a patient to palliative care services, but this doesn’t always mean end-of-life care. Today people can be referred to these services much earlier if they’re living with cancer. Palliative care can help one to live as well as possible including managing pain and symptoms. This care may be at home, in a hospital or at another location one prefers. Additional supportive care (treatment or services that support you through a cancer experience) are also available.
Traditional Māori Healing | Rongoā Māori
Rongoā Māori is a body of knowledge that takes a holistic view to wellbeing and treatment. In particular, it focuses on hinengaro (mind), wairua (soul), mauri (life essence), ngā atua (Gods) and te taiao (the environment).
There are many providers who are able to provide rongoā services. Your Māori Health team at the hospital will be able to connect you with one nearest to where you live.
See the below websites for more information on rongoā Māori
Other complementary therapies
Complementary therapies are treatments that are used alongside standard treatments. They are often used to boost the immune system, relieve symptoms, and enhance the effectiveness of standard treatments.
Speak to your doctor if you intend to use complementary therapies to ensure that they will work well alongside your treatment.
Some examples of complementary therapies are:
acupuncture
meditation and mindfulness
music therapy
massage
aromatherapy
naturopathy
tai chi
pilates
visualisation or Guided Imagery
spirituality
Click here to find out more about complementary therapies
Side Effects from Treatment
Ngā mate āpiti

Side effects of stomach cancer treatment | Ngā mate āpiti o te rongoā mate pukupuku puku
As with any medical treatment, you may experience side effects from your cancer treatment. This is perfectly normal and can be a sign that the treatment is working, although it may feel unpleasant. Side effects vary from person to person and depend on the type of treatment, the part of the body treated, and the length and dose of treatment. Most side effects are temporary and go away after treatment ends. Below you can find information on some common side effects of treatments and how you can manage them to improve your daily well-being.
You may experience side effects other than those discussed here.
If you experience side effects, let your healthcare team know when you next see them. If the symptoms feel extreme or are worrying you, get in contact with your oncology team sooner.
Common side effects of stomach cancer treatments | Ngā mate āpiti tōkau o te rongoā mate pukupuku puku
Click on each treatment to learn more about the side effects of that treatment | Pāwhirihia i ia momo rongoā kia tirohia i ngā mate āpiti e hāngai ana
Surgery | Poka tinana
Some side effects of surgery are due to the anaesthesia and should fade shortly after the surgery. These include:
nausea | whakapairuaki
vomiting | whakaruaki
dizziness | takaānini
agitation | pōkeka.
Other side effects are due to the surgical procedure itself which should subside shortly after surgery. These include:
fatigue | ruha
pain at the site of the surgery | mamae wāhi poka.
Some additional side effects may present due to the disruption to your digestive system as a result of the surgery and could take weeks or months to recover from.
These include:
diarrhoea and malabsorption | kotere me whākapi miti
weight loss | heke taumaha
loss of appetite | minangaro
feeling full quickly | pūnaunau wawe.
Chemotherapy and biological therapies | Haumanu matū, koiora
Chemotherapy treatment kills cancer cells, but in the process, damages normal healthy cells which causes side effects. These side effects vary from person to person and depend on the type of treatment, the part of the body treated, and the length and dose of treatment. Below are some common side effects of this.
nausea and vomiting | whakapairuaki & whakaruaki
loss of appetite | minangaro
feeling full quickly | pūnaunau wawe
diarrhoea and constipation | kotere me te kōroke
fatigue | ruha
weight loss | heke taumaha
sore mouth or throat | mamae o te waha/ korokoro
taste changes | panonitana rongo tawara
hair loss | whakahewa
dry or itchy skin | kiri mangeo
foggy brain.
Some chemotherapy side effects can be life threatening therefore it is important to go to contact your oncology team or go to your nearest emergency department immediately if you experience any of the following and let them know that you are undergoing chemotherapy treatment. These include:
fever or chills
rain in your chest or difficulty breathing
diarrhoea
vomiting that is not eased with anti-sickness medication
bleeding from the gums or nose that doesn’t stop
pain or blood present when passing urine.
Radiation therapy | Haumanu iraruke
Radiation therapy is used to kill cancer cells, but it can also kill some healthy cells near to the cancer site too. Although radiation therapy itself does not hurt, you may experience some symptoms afterwards due to the affect the radiation has on the healthy cells. These symptoms may include:
nausea and vomiting | whakapairuaki & ruaki
loss of appetite | minangaro
feeling full quickly | pūnaunau wawe
diarrhoea and constipation | kotere & kōreke
fatigue | ruha
similar to a sunburn - at the radiation site | mamae tīkākā
weight loss | heke taumaha.
Managing symptoms and side effects | Whakahaere tohumate me ngā mate āpiti
Click on the symptoms below to find information on how to manage symptoms and side effects | Pāwhirihia i ia momo tohumate mō ngā mōhiohio kia whakahaere ai ngā tohumate me ngā mate āpiti
Fatigue | Ruha
A common side effect of treatment is feeling constant tiredness (fatigue). Treatment or the cancer itself can reduce the number of red blood cells in your body, resulting in anaemia, which can make you feel very tired.
Tips to manage fatigue | Ngā kupu āwhina mō te whakahaere i te ruha:
Use your energy wisely
plan ahead for when you feel too tired to cook
shop online for groceries
bulk cook meals you can store in the freezer
cook when you have more energy
ask and accept offers of help with shopping and cooking from whānau and friends
use home delivery services such as Meals on Wheels or other companies that bring pre-prepared food to you. You can ask for help to access these via your social worker
keep snacks handy in your bag or car.
Activity can help with fatigue
regular, gentle exercise can help improve fatigue and your appetite
activity can mean many things – walking, stretching, even vacuuming!
set small goals. Set a timer for five minutes and see what you can manage in this time
eat with others.
Loss of appetite | Kore hiakai
It can be discouraging to lose your appetite. You may lose your appetite because of the effects of cancer itself, the treatment, or other side effects, such as feeling sick, not enjoying the smell of food, or feeling upset. To help you can:
eat small amounts often, e.g., every 2–3 hours. Keeping to a regular eating pattern rather than waiting until you are hungry will mean your body gets the nourishment it needs to
use a smaller plate – a big plate of food may put you off
eat what you feel like when you feel like it. Have cereal for dinner or a main meal at lunch
include a variety of foods in your diet
sip fluids throughout the day
replace water, tea and coffee with drinks or soups that add energy (kilojoules/calories), such as milk, milkshake, smoothies, replacement drinks or soup
relax dietary restrictions – maintaining your weight or regaining weight you have lost is more important than avoiding full-fat and other high-energy foods
gentle physical activity can stimulate appetite – take a short walk around the block
eat with others
keep snacks handy e.g., in your bag or car so you can eat on the go
talk to your dietitian about liquid meal replacements that might be easier to digest.
Taste or smell changes | Rongo kakara me te hā
Some treatments such as chemotherapy can change the way food and/or drink taste or smell. It may taste bland or metallic.
Tips on managing changes in taste include:
add extra flavour to food if it tastes bland – like fresh herbs, lemon, lime, ginger, garlic, soy sauce, honey, chilli, or pepper
experiment with different food, as your tastes may change
if meat tastes bad during treatment, replace it with other protein sources like cheese, eggs, nuts, dairy foods, baked beans, lentils, or chickpeas
add small amounts of sugar to food if it tastes bitter or salty
use a straw when drinking
change from using metal cutlery to plastic or bamboo cutlery.
Tips on managing changes in smell include | Ngā kupu āwhina mō te whakahaere i ngā panoni rongo kakara:
eat cold food or food at room temperature (hot food smells more)
reheat pre-prepared meals in the microwave so the cooking smell doesn’t put you off
stay out of the kitchen, if possible, when food is being prepared
ask family or friends to cook
use the exhaust fan, open the kitchen window, or cook outside to help reduce cooking smells.
Nausea and vomiting | Whakapairuaki me te ruaki
Feeling sick and vomiting are often side effects of cancer, its treatment, or some medicines. They often occur together, but not always.
Nausea | Whakapairuaki
Nausea is stomach discomfort and the sensation of wanting to vomit. Nausea can be a precursor to vomiting the contents of the stomach and may be caused by treatment, stress, food odours, gas in the gastrointestinal tract, motion sickness or even the thought of having treatment.
Tips on how to cope with nausea | Ngā kupu āwhina ki te morimori i te whakapairuaki:
have a light snack before treatment and wait a few hours before eating again
eat small meals 5–6 times during the day. Going without food for long periods can make nausea worse
snack on dry or bland foods, e.g., crackers, toast, dry cereals, bread sticks or pretzels
choose cold foods or foods at room temperature instead of hot, fried, greasy, or spicy foods
eat and drink slowly and chew your food well
try foods with ginger, e.g., ginger biscuits, or ginger beer
avoid foods that are overly sweet, fatty, fried, spicy, or oily, or that have strong smells
brush teeth regularly to help reduce unpleasant tastes that may make you feel nauseated
do not eat your favourite food when feeling nauseated to avoid developing a permanent dislike
suck on hard lollies – flavoured with ginger, peppermint, or lemon
try ginger food and drink items, such as candied ginger, ginger beer, ginger ale, or ginger tea. Talk to your dietitian doctor or pharmacist about ginger supplements
take anti-nausea medicines as prescribed. Let the doctor know if the medicines don’t seem to be working.
Vomiting | Ruaki
Vomiting is the forcible emptying (“throwing up”) of stomach contents through the mouth. Vomiting can follow nausea and may be caused by treatment, stress, food odours, gas in the gastrointestinal tract, motion sickness or even the thought of having treatment.
Vomiting is more serious than nausea. Vomiting can cause dehydration and increase the risk of malnutrition. See a doctor if you are vomiting for more than one day, especially if you cannot keep water down as you may become dehydrated.
Tips on how to cope with vomiting | Ngā kupu āwhina ki te morimori i te ruaki:
Take small sips of water or clear liquids, such as ginger ale, soda water or sports drinks like Gatorade or Hydrolyte. Dilute sweet drinks. If you feel like a fizzy drink, open it, and let it sit for 10 minutes or so, and drink it when it’s a bit flat
sucking on crushed ice cubes or an ice block can be soothing
once you can keep clear liquids down try some different drinks, such as consommé and clear broths, weak tea, herbal tea, fruit drinks, beef, and chicken stocks
have small, frequent meals and snacks throughout the day
introduce bland, starchy foods, such as plain biscuits, bread or toast with honey or jam, peanut butter, rice, yoghurt, or fruit. Attempt small, frequent servings at first
consume a little bit more each time until you are eating a well-balanced diet.
Chewing and swallowing | Ngaungau me te horomi
After treatment chewing and swallowing may be difficult and painful. Surgery, radiotherapy, and chemotherapy can cause temporary problems. People with dentures who have lost weight may also find their teeth become loose, which can make eating difficult.
Signs that you are having problems with chewing and swallowing include taking longer to chew and swallow, coughing or choking while eating or drinking, or food sticking in your mouth or throat like a ball.
Tips on chewing and swallowing | Ngā kupu āwhina mō te ngaungau me te horomi:
change how you prepare your food by chopping food up into smaller pieces or pureeing
let your doctor know that you are having issues and get a referral to see a speech pathologist and dietitian
a speech pathologist can monitor your ability to swallow and suggest modifications to the texture of your food once your ability to swallow and chew begins to improve. A dietitian can ensure you are meeting your nutritional needs.
Mouth changes | Ngā panonitanga o te waha
Some chemotherapy drugs and some pain medicines can make your mouth dry, cause mouth ulcers, or change the amount of saliva in your mouth. A dry mouth can increase the risk of tooth decay and infections such as oral thrush, which will make eating harder.
Ulcers may also be present in your digestive tract, causing discomfort in the stomach or bowel and diarrhoea.
Tips to lessen discomfort with mouth sores | Ngā kupu āwhina ki te whakamauru i ngā harehare waha:
suck on ice cubes
eat soft foods – stews, soups, scrambled eggs, and smoothies
cold foods and fluids may be more comfortable than hot ones
avoid ‘coarse’ foods that can irritate your mouth, such as crackers, toast, nuts, and seeds
avoid spicy or very hot foods
use a straw and direct liquids away from the areas where mouth sores are most painful
talk to your doctor about medication or mouth washes to help manage the pain and allow you to eat more comfortably.
Tips to relieve a dry mouth | Ngā kupu āwhina ki te whakamauru i te waha maroke:
suck on ice cubes
keep your mouth clean with regular mouthwashes to prevent infections
gargle with 1⁄2 tsp salt or 1 tsp bicarbonate of soda in a glass of water
choose an alcohol-free mouthwash to avoid irritating your mouth further
use a soft toothbrush when cleaning your teeth
ask your dentist or health care team about suitable mouth rinses or oral lubricants
limit alcohol and coffee as these are dehydrating fluids and avoid smoking
avoid ‘coarse’ foods that can irritate your mouth, such as crackers, toast, nuts, and seeds
avoid spicy or very hot foods
soften food by dipping it into milk, soup, tea, or coffee
moisten with sauce, gravy, cream, custard
sip fluids with meals and throughout the day
chew sugar-free gum to stimulate the flow of saliva.
Changes in bowels- constipation and diarrhoea | Ngā panonitanga o ngā kōpiro
Living with cancer and its treatments can result in changes to your bowel habits. This could be differences in the appearance, consistency, and/or the smell of your stools.
Constipation | Kōroke
This is when your bowel motions are infrequent and difficult to pass. It can be caused by different factors including regularly taking opioid medicines; having a diet low in fibre; not getting enough exercise; not having enough fluids to drink (dehydration); or having a low overall food intake.
Tips on how to manage constipation | Ngā kupu āwhina mō te whakahaere kōroke:
soften stools by drinking 8–10 glasses of fluid a day, e.g., water, herbal tea, milk-based drinks, soup, prune juice
eat foods high in fibre, e.g., wholegrain breads, cereals, or pasta; raw and unpeeled fruits and vegetables; nuts and seeds; legumes and pulses
if you are increasing the amount of fibre in your diet, increase fluids to prevent the extra fibre making constipation worse
ask your doctor about using a laxative, stool softener and/or fibre supplement
exercise – check with your doctor, exercise physiologist or physiotherapist about the amount and type of exercise that is right for you.
Diarrhoea | Kotere
This means your bowel motions are watery, urgent, and frequent. You may also get abdominal cramping, wind, and pain. Frequent loose stools can occur because you are not digesting food or absorbing nutrients properly. Cancer treatment, medicines, infections, reactions to certain foods and anxiety can all cause diarrhoea.
Diarrhoea can result in dehydration, so it’s important to stay hydrated by drinking extra fluids. Every time you have a loose bowel movement you should drink an extra cup of non-caffeinated fluid. If you have diarrhoea for several days, see your doctor so he/she can determine the cause and help to manage your diarrhoea. Your doctor may decide to prescribe you anti-diarrhoea or over-the-counter. medication.
Tips on how to manage diarrhoea | Ngā kupu āwhina mō te whakahaere kōtere:
drink plenty of fluids to avoid becoming dehydrated. Water and diluted cordials are better than high-sugar drinks, alcohol, or caffeinated fluids – remember signs of dehydration are smaller amounts of dark urine
choose low-fibre foods, e.g., bananas, mashed potato, rice, pasta, white bread, oats, steamed chicken without the skin, white fish
avoid foods that increase bowel activity, e.g., spicy, fatty, or oily foods, caffeine, alcohol, or artificial sweeteners
try soy milk or lactose-free milk if you develop a temporary intolerance to milk (lactose)
don’t eat too many raw fruit and vegetable skins and wholegrain cereals as they may make diarrhoea worse
avoid foods and drinks that are high in sugar, such as cordial, soft drinks and lollies
avoid foods sweetened with artificial sweeteners such as sorbitol, mannitol, and xylitol. These are often marketed as ‘sugar-free’
it may also help to eat small, frequent meals throughout the day, rather than three large meals.
Heartburn (Indigestion) | Tokopā
Some cancers and treatments can cause heartburn, which is a burning sensation in the upper chest, oesophagus and/or throat. It is caused by the contents of the stomach coming back up into the oesophagus (reflux).
Heartburn may make you feel too uncomfortable to eat much, which could lead to weight loss. If the tips below do not relieve heartburn, let your doctor know as medication may help to prevent or manage these side effects.
Tips to manage heartburn | Ngā kupu āwhina mō te whakahaere tokopā:
avoid large meals; try to eat 3 small meals and 3 small snacks throughout the day
eat slowly and take the time to enjoy your meal
avoid wearing tight clothing while eating, especially belts
sip fluids between meals, rather than drinking large amounts at mealtimes
limit or avoid foods that may make heartburn worse, e.g., chocolate, highly seasoned spicy foods, high-fat foods (e.g., fried food, pastries, cream, butter, and oils), tomato and tomato products, citrus fruits, coffee (including decaf), strong tea, soft drinks, and alcohol
straight after eating, sit upright for at least 30 minutes and avoid lying down or activities that involve bending over (e.g., gardening).
Peripheral neuropathy | Pūtau Iotaiaki mōwaho:
Peripheral neuropathy is caused by damage to the peripheral nerves. These are the nerves in the body outside the brain or spinal cord. Peripheral neuropathy may be caused by cancer, cancer treatments or other health problems. It most commonly affects the hands and feet. Peripheral neuropathy caused by cancer treatment will get better over time with proper treatment and care.
The most common symptoms of peripheral neuropathy can include | Ngā kōrero tōkau mō te Pūtau Iotaiaki Mōwaho:
tingling, burning, numbness or pain in the hands or feet
difficulty doing up buttons and picking up small items
loss of feeling especially in the hands and feet
problems with balance or walking, and clumsiness
be safe. If you notice changes in your walking, stance, fine and gross motor skills, or balance speak to your doctor as soon as possible and ask for a referral to an occupational therapist, exercise physiologist or physiotherapist.
Tips to manage peripheral neuropathy | Ngā kupu āwhina mō te whakahaere Pūtau Iotaiaki Mōwaho:
use a night light so that you don’t trip or bang into anything if you need to go to the toilet at night
keep clutter and rugs off the floors
have clear paths to the toilet and bedroom
use handrails where possible
use nonslip mats in the shower and bathroom
be careful on slippery and wet floors
do not walk around bare footed as you may not notice if you stand on something that could damage your feet
wear shoes and slippers that fit well
use a walking stick if you need to
wear gloves when washing up, cleaning and gardening
test water temperature with your elbow
take care when cutting food and opening cans or jars
keep your skin moisturised to prevent cracking
check your hands and feet daily for signs of injury, rubbing, redness or infection
ask for help if you need it, e.g., to do up buttons and shoes
find clothes and shoes that are easy to put on and take off
avoid driving if symptoms are severe.
Alerting your healthcare team of side effects | Whakaohititia tō rōpu tiaki hauora ki ngā mate āpiti
Your health care team wants to hear about your side effects. Your questions and concerns are important. Do not be afraid to share them. Ask your health care team who you should contact if you feel that your side effects need assessing right away.
Treatment changes | Ngā pānonitanga maimoa
Occasionally, if you have severe side effects, your doctor may discuss delaying or changing your treatment to prevent further discomfort.
Start a symptom diary | Tīmatahia he rātaka tohumate
Keeping track of your symptoms can help you and your cancer care team to manage them better.
Know who to contact if you have a problem | Me mōhio hoki ki te whakapā atu ki a wai mēnā he raru tāu
Ask your doctor or nurse:
when you should call for help or advice
who you should contact
how to contact them (including at night or weekends).
Keep this information where you can easily find it.
Our partners at the Pancare Foundation have created a webinar to help patients manage these side effects and help you navigate each day and experience greater quality of life. Pancare's experts share their knowledge surrounding common side effects such as nausea, peripheral neuropathy, fatigue, mouth sores, abdominal discomfort and more. Practical ways to manage these side effects are explored along with information regarding the support and care available for you and your family.
*NB - The PanSupport service mentioned is not available to patients in New Zealand
Diet & Nutrition
Whiringa kai me te taioranga

Why is diet and nutrition important? | He aha e whaitikanga ai te whiringa kai me te taioranga?
You may be feeling that some things are out of your control, however there are a number of actions that you can take to make sure your body is in the best condition to cope with, and heal from, the symptoms and side effects of the cancer and cancer treatments.
Below you will find detail about why diet and nutrition can make a big difference to the healing process and how you feel.
Why does stomach cancer affect nutrition? | He aha e pāngia ai te mate pukupuku kōpiro i te taioranga?
Stomach cancer, and cancer treatments place extra demands on your body. They can also cause you to lose your appetite and energy, putting you at an increased risk of malnutrition. It is important to ensure that your body is receiving the right nutrition before, during and after treatment to be able to cope with these extra demands.
Your food choices when you have cancer and are undergoing treatment may be very different from what you are used to eating.
The main goal is to try to keep your weight constant, maintain muscle strength, maintain a healthy weight, and have more energy, all of which help your body to heal properly, improve your quality of life and give you the energy to cope with all the new challenges treatment may bring.
Stomach cancer and the treatments for stomach cancer may impact | Ka pāngia pea te mate pukupuku puku me ngā rongoā:
your nutritional requirements and what you need to eat
how much you eat
your appetite
your ability to digest food
your ability to maintain your weight and muscle mass
your energy levels and general wellbeing.
Good nutrition can help to | E āwhina ai te taioranga pai ki te:
manage the side effects of treatment
speed up recovery after treatment
heal wounds and rebuild damaged tissues after surgery, radiotherapy, chemotherapy, or other treatment
improve your body’s immune system and ability to fight infections.
Overall, try to make food choices that provide you enough | Heoi, kia whakamātau koe ki te whiriwhiri i ngā kai e ratoa ai:
calories (to maintain your weight)
protein (to help rebuild tissues that cancer treatment may harm)
nutrients such as vitamins and minerals
fluids (essential for your body’s functioning).
Exercise can also help with appetite and digestion issues related to treatment.
Nutritional tips during treatment | He kupu āwhina taioranga e koke ai te maimoatanga
Click here to learn more about nutritional tips during treatment | Pāwhirihia ki kōnei mō ētahi atu whakamōhiotanga
To maintain good nutrition:
you may need more energy (kilojoules/calories)
eat small, frequent meals or snacks, rather than three large meals a day
ask for a referral to a dietitian – discuss eating issues, weight issues, muscle loss
do some light physical activity, such as walking, to improve appetite and mood, reduce fatigue, help digestion, and prevent constipation
check with your doctor or dietitian before taking vitamin or mineral supplements or making other changes to your diet
relax dietary restrictions, e.g., choose full-cream rather than low-fat milk
consider using nutritional supplements if you cannot eat enough – discuss options with your doctor, palliative care specialist or dietitian.
Nutritional tips following surgery | Ngā kōrero āwhina taioranga whai muri i te pokanga
Click here to learn more about nutritional tips following surgery | Pāwhirihia ki kōnei mō ētahi atu whakamōhiotanga
Surgeries used to treat cancer may result in a variety of side effects, including weight loss and diarrhoea. The side effects usually only last for a short period of time, but you may have to make some changes to your diet to ensure that you are getting enough nutrition and maintaining your weight.
Your body needs good nutrition after surgery, and it is an important part of your recovery process. If you are struggling to eat or drink, the hospital may prescribe nutrition supplements, or recommend tube feeding, to help you to maintain weight and provide you with the nutrients you need for speedy recovery.
Tips on maintaining weight after surgery | Kupu āwhina kia ū te taumaha whai muri i te pokanga:
monitor your weight – weigh yourself once or twice a week to monitor for any weight loss
if you are losing weight, tell your doctor and get a referral to see a dietitian
eat small, frequent meals after surgery so your digestive system only has to deal with a small amount of food at a time.
Feeding tubes | Ngongo whāngai kai
Some patients have trouble taking in enough nutrition after surgery for stomach cancer. Further treatment like chemotherapy with radiation can make this problem worse. To help with this, a tube can be placed into the intestine at the time of gastrectomy. The end of this tube remains outside of the skin on the abdomen. Through this, liquid nutrition can be put directly into the intestine to help prevent and treat malnutrition.
Below are some tips to keep healthy if you have a feeding tube | Kupu āwhina kia ū te hauora ki te whakamahi ngongo whāngai kai:
check type of tube feed is right for your needs
follow the hygiene rules, wash hands before and after feeds, keep syringes & equipment clean & dry
check that the feeding tube is in the right position before feeding – your care team will show you how to do this
flush the tube through before and after adding the feed (or medication) to avoid blockages – follow the instructions provided by your dietitian
position yourself in an upright position when feeding
clean around the insertion site every day
look after the skin around the tube to avoid irritation
make sure that you stay hydrated by having water through the tube (speak to your dietitian to discuss how much water you can use) or orally if safe, appropriate, and agreed with healthcare team
keep your teeth and gums healthy by cleaning teeth twice a day even if you are not feeding or drinking through the mouth.
Click here to see a diagram of a feeding tube | Pāwhirihia ki kōnei kia tirohia he hoahoa o te ngongo whāngai kai
Nutritional tips to prevent Dumping Syndrome | Kupu āwhina taioranga kia aukati i te mate tātuku kōpiro
Click here to learn more about nutritional tips to prevent Dumping Syndrome | Pāwhirihia ki kōnei mō ngā kōrero āpiti
Removal of the lower part of the stomach can result in a condition called Dumping Syndrome.
Dumping syndrome can occur when food moves from the stomach into the small bowel too quickly.
Symptoms of dumping syndrome (1-3 hours after eating):
nausea
cramps and diarrhoea approximately 10-30 minutes after eating or sweating
dizziness.
Tips to prevent Dumping Syndrome include:
avoid large meals
avoid sugary drinks and sweets
choose meals high in protein to slow the digestion of carbohydrates
keep drinks separate to meals.
We recognise that dietary changes have a huge impact on everyone with cancer. It can take a while to get used to changes to your diet and lifestyle but finding ways to manage your diet and symptoms can help you feel more in control. It can also be helpful to speak to your dietitian, doctor or nurse.
Living well with cancer
Kia ora pai ai

Learn more about living with cancer.
Read about other people’s cancer journeys see our personal journeys page.
Useful Websites & Patient Support | Ngā pae tukutuku whai take me ngā wāhi āwhina tūroro
DISCLAIMER: Information provided by the Gut Cancer Foundation should be discussed with your healthcare professional and is not a substitute for their advice, diagnosis, treatment, or other healthcare services. In some cases, information has been gathered from international sources and should be discussed with New Zealand health care professionals.







