Your medical team are the ones who are there to provide direct clinical care and treatment. They are the ones who can provide advice on what the best options are for you and provide those treatments either in the hospital or clinic in the community.
There is usually one person who will be the central communicator to relay information about your care to other members of the team. This is usually your oncologist or GP. When you go to your next appointment, ask who your key contact is if you don’t know.

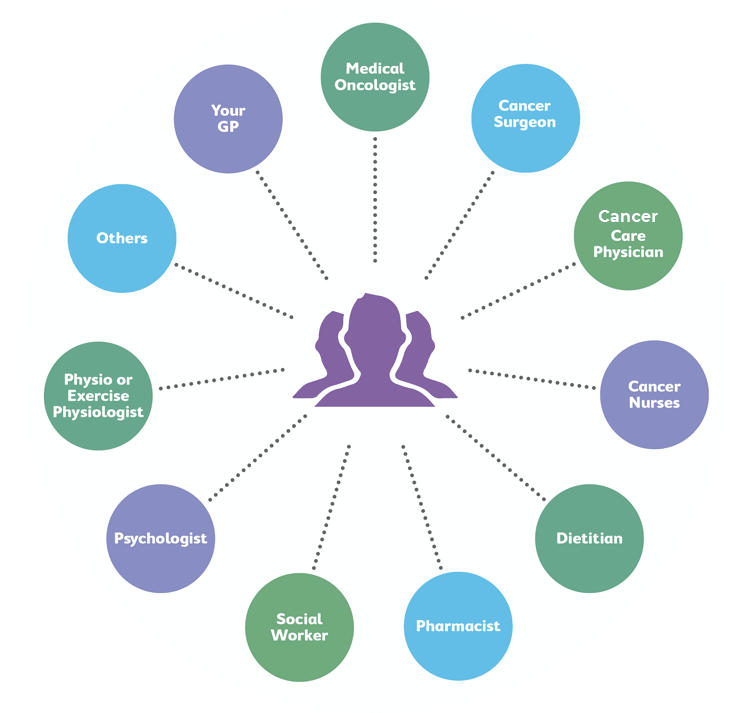
Depending on your treatment, your treatment team may consist of a number of different health professionals, such as:
general practitioner – your GP looks after your general health and works with your specialists to coordinate treatment.
gastroenterologist – specialises in diseases of the digestive system, can also perform endoscopy procedures.
upper gastrointestinal (UGI) surgeon – specialises in surgery to treat diseases of the upper gastrointestinal system.
medical oncologist – prescribes and coordinates chemotherapy treatment.
radiation oncologist – prescribes and coordinates radiation therapy.
cancer nurses – assist with treatment and provide information and support throughout your treatment.
other allied health professionals – such as dietitians, exercise physiologists, social workers, pharmacists, speech pathologists and counsellors.
Your care team may work in the hospital, in clinics in the community, or even come to your home. Their role may be to advise on and provide treatment; help you with the symptoms and side effects of cancer and cancer treatments; or be there to support you in making sure you are living as comfortable and fulfilling life as possible.
This diagram gives an example of who might be part of your care team.
Communicating with your medical care team
Good communication between you and your treating team is very important.
You should expect to:
understand your health condition and plans for your treatment
be able to ask any question that you want answered
know who the members of your treating team are
know who your contact person in the team is in case you have questions
have clear, open and respectful communication with all health staff
be able to request copies of your tests and reports if you wish to have them
ask how experienced a health professional is with treating pancreatic cancer
seek second or third opinions if you want to
negotiate a break in your treatment if you believe you need it
have someone ask you about your needs for support.
You can learn more about your rights and what to expect when receiving health care on the Health and Disability Commission Website.
A cancer diagnosis can be overwhelming and confusing as there is a lot of information to digest.
If you can, take someone with you to medical appointments.
Being given a lot of information can be overwhelming so a friend or family member can be a second pair of ears. If English is not your first language, try to take an English-speaking family member or friend with you – even when an interpreter is available.
Here you can find some questions that you might want to download to ask your oncologist at your next appointment. It is important to ask every question that you want answered.
Some questions you may ask are:
what is the specific type of cancer, has it spread and what are the recommended treatment options? For example, surgery, chemotherapy or radiotherapy.
where the treatment will take place and what are the side effects?
the impact of cancer treatment on diet. Will I need to see a dietitian?
what will be the cost of the treatment and medicines and if these can be reduced?
are any clinical trials suitable for me?
what are the ways to complement medical treatment such as rongoā Māori, massage, exercise or meditation?
are there other things such as emotional and practical support I might need?
when will palliative care be suggested?
what does this diagnosis mean for my future?
Below you can find some additional questions you might want to ask:
Shared decision making
what is my diagnosis?
what are the likely outcomes of this diagnosis and what is my chance of recovery?
Optimal care
do you specialise in treating my type of cancer?
has this treatment been successful for my diagnosis?
what are the outcomes or complications you have faced with my type of cancer?
is there anything unique about my cancer that makes my prognosis better or worse?
Is there another specialist who treats this type of cancer that you recommend for a second opinion?
Care plan
Will a written plan of care be provided?
Will this plan include:
the frequency of treatments and tests
side effects I should expect and how to manage them
disruptions to expect to my work, family or other responsibilities
resources I can use to understand my diagnosis and treatment better
how and when to contact my care team if I have questions or concerns
how my caregivers will be involved and my preferences for how I would like to be treated
will a member of my care team provide a clear explanation of my care plan so that I can understand it?
Holistic care
Will someone need to drive me to treatment(s)?
Is help available if transportation is an issue?
Do you have any information around diet, exercise or other health recommendations?
How will any medication I am currently taking interact with my treatment?
Will you schedule all my necessary appointments and provide a copy for my reference?
Emotional and mental health
is there support or counselling available for emotional or psychological concerns (anxiety, depression or other worries) I may have?
do I require a referral to speak with counsellor?
Treatment options
is it necessary to have treatment right now?
what are all my treatment options?
what are the pros and cons of each treatment option?
what is the goal of this treatment?
how will I know if my treatment is working?
what are the side effects of my treatment?
how can I prepare for the side effects of my treatment or prevent them?
are there any alternative treatment options available to me?
how will treatment affect my daily activities?
how will treatment affect my quality of life?
what can I expect if I decide not to have treatment?
how much time do I have to think about this? Do you need my decision today?
what is your opinion about the best treatment for me?
Treatment plan
what exactly will be done during the treatment and how will it affect me?
what is the treatment schedule, e.g. how many treatments, how often, and for how long?
where will I have the treatment?
are there any advantages/disadvantages of the private versus public health system?
Preparing for treatment
is there anything that I can do before or after my treatment that might make it more effective? For example, diet, work, exercise?
what are the do’s and don’ts while having treatment?
what problems should I look out for and who do I contact if they occur?
what is my long-term follow up plan?
What are clinical trials?
what are clinical trials?
are there any clinical trials that I may be suitable for?
what are the pros and cons of clinical trials?
what is involved if I enrol in a trial (extra appointments, questionnaires)?
Costs
what will be the costs throughout my treatment, e.g. medication, chemotherapy, etc?
am I eligible for any benefits if I cannot work?
can I change from Public hospital treatment to Private hospital?
can I change from Private hospital treatment to Public hospital – can you arrange this? Will I need another referral?
Multidisciplinary team
what is a multidisciplinary team?
do you work as a part of a multidisciplinary team?
can you explain the advantages of a team approach?
how do you all communicate with each other and me?
who will oversee my care?
what do I do if I get conflicting information?
Advanced stage cancer
Finding out that you have advanced cancer, or a recurrence of your disease can feel overwhelming. The questions listed here may help you to understand your condition and the treatments you are being offered.
what is palliative care?
do I need a referral to access palliative care?
what other treatment options are available to me?
when is a good time to stop treatment?
how can I effectively plan my end of life care?
what support is available to me and my family for managing advanced stage cancer?
are there any other professionals or specialists who I should be referred to?
do I need a referral into palliative care?
Asking for a second opinion can feel uncomfortable and awkward however be reassured that it is not unusual.
Second opinions are requested for a variety of different reasons. Some people seek a second opinion because they want to have peace of mind that they have explored all options and opinions available before starting treatment. Some people may have heard about a treatment and want another doctor’s opinion about it. Some people feel that the communication with their doctor is difficult and they would like to speak to someone who may have a different approach.
If you do want a second, or even third, opinion, make sure to let your GP know in advance so that they can share any tests or assessments that have been done so far.
You can seek a second opinion by either:
asking your Oncologist
asking your GP to refer you for a second opinion.
It is also a good idea to check with your GP or Oncologist whether seeking a second opinion would delay treatment.
Below is an example of how you might start the conversation with your doctor to request a second opinion.
“I think I would like to seek a second opinion to make sure that I have covered all my bases before starting treatment. Can you help me with that?”
Telehealth appointments are appointments that are undertaken over the phone or on video with you.
Telehealth appointments can be a great way to meet with your care team if the appointment is a short, routine and straightforward one and you live far away from the clinic. Not all appointments will be able to be undertaken via telehealth though.
What are the benefits?
Telehealth provides a safe way to meet during COVID-19 and can, more generally, be helpful to:
enable you to continue your vital health care
reduce your risk of getting other illnesses like colds, flu and Coronavirus. This is important if your immune system (your body’s ability to fight infection) has been weakened by your cancer treatment
avoid the need to travel to appointments
save you money on travel and accommodation costs
be faster if you just need a prescription or have a quick question for your treatment team.
What appointments are best for telehealth?
During your cancer treatment, you will need to see various health professionals. Telehealth is best for the following types of appointments:
follow-up care
scan and test results
advice on symptoms and side effects
repeat prescriptions
nutrition and exercise advice
counselling
You may have a choice between phone and video telehealth appointments. Speak with your care team to understand their offerings and let them know your preferred mode of telehealth appointment. Your health professional will tell you if they need to see you in person and will arrange follow-up appointments.
What set up do I need?
Phone calls:
a mobile phone or landline.
Video calls:
a smartphone, iPad/ tablet, laptop or a computer that has a camera, microphone and speakers
an email address or mobile phone number so they can email or text you the instructions and link
Internet connection.
Note: Not all health professionals will have the technology to conduct video calls. In these situations, consultations will be done via phone.
Preparing for your telehealth appointment:
Check with your health professional if you are able to see or access scan or test results.
Let your health service know if you:
are hard of hearing
need an interpreter.
Make sure you:
read any instructions
have a list of questions prepared
have the email address for your local pharmacy so if you need a prescription your doctor can email the pharmacy any prescriptions
have a support person attend if needed. Find a quiet place so you won’t be interrupted and make sure you don’t have a window or light behind you
do not have your mobile phone on silent
turn your microphone on (off mute) and your camera is on if you’re using a laptop or tablet (iPad)
rest your screen on something so you don’t have to hold it. This will make it easier for you to concentrate on the call and will also free your hands to write any notes. A pile of books on the kitchen table can work well
set up the screen so you have your face and shoulders in view
connect a few minutes before your appointment time so you can check everything is working ok.
During the appointment:
Look at the screen.
Speak slowly and clearly.
Take it in turns to speak one at a time. Do not talk over each other. If you get cut off, wait for a phone call from your health professional.
Write down any instructions and what you need to do next.
Ensure you have asked all your questions.
Ask your doctor if they can share their screen with you when they are going through test or scan results.
Can I ask for a face-to-face appointment?
Yes, you can and should ask your health care provider for a face-to-face appointment. You should have a face-to-face appointment if:
it is your first time seeing the doctor
your health professional has asked to see you in person. They will tell you how to stay safe when visiting
you are not getting better.
Or if you:
need a physical examination, test, treatment or scan
do not feel comfortable using telehealth
do not have the technology or cannot use it
have more than one appointment at the health centre or hospital.
Can I have a support person with me for the appointment?
Yes. Just make sure you introduce the person to the health professional at the start of the call/ video as you would if you were meeting in person.









